When your doctor prescribes a bioequivalent medication, you might wonder: is this really the same as the brand-name drug? Many people think generics are inferior, but the truth is more nuanced. Bioequivalence isn’t about chemical identity-it’s about how your body processes the drug. Let’s break down what this term really means.
What Bioequivalence Really Means
Bioequivalence is a precise scientific term used to determine if two medications deliver the same amount of active ingredient to your bloodstream at the same rate. According to the U.S. Food and Drug Administration (FDA), it means "the absence of a significant difference in the rate and extent to which the active ingredient becomes available at the site of drug action" when tested under controlled conditions. This isn’t about the drug looking identical-it’s about your body responding the same way.
The World Health Organization (WHO) defines it similarly. Both agencies agree: two drugs are bioequivalent if they produce the same therapeutic effect. For example, a generic version of the blood pressure medication lisinopril must release the same amount of drug into your blood within the same timeframe as the brand-name version. This ensures the generic works just as well.
How Bioequivalence Is Tested
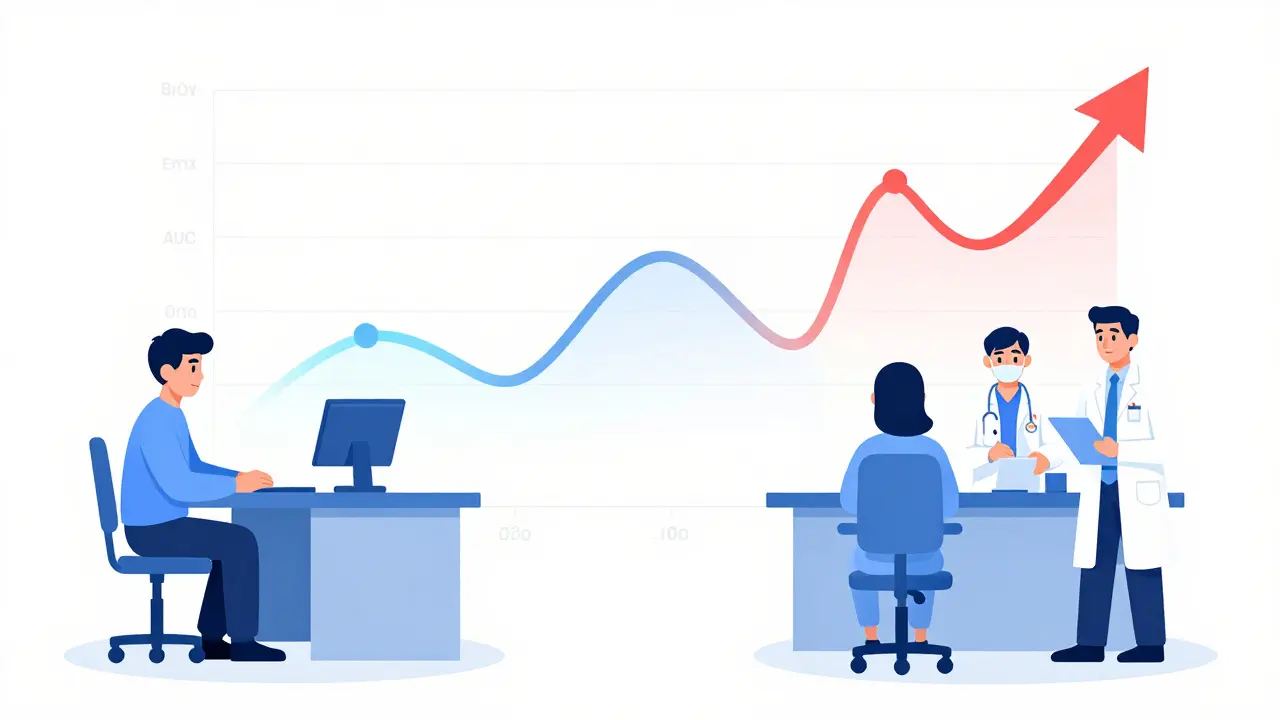
Testing bioequivalence isn’t guesswork. It’s done through clinical studies with healthy volunteers. Researchers measure three key things:
- Cmax: The highest concentration of the drug in your blood.
- tmax: How long it takes to reach that peak level.
- AUC: Total drug exposure over time (area under the curve).
The FDA requires that for a generic drug to be approved, these measurements must fall within 80% to 125% of the brand-name drug’s values. Why this range? Because a 20% difference in drug exposure is statistically unlikely to affect most treatments. For instance, if a brand-name drug has an AUC of 100 units, the generic must show between 80 and 125 units. This isn’t arbitrary-it’s based on decades of real-world data.
Studies typically involve 24 to 36 volunteers. They take the brand and generic drugs on separate occasions, with blood samples taken over hours to track drug levels. The FDA only approves generics if the data consistently meets these standards. For drugs with a narrow therapeutic index (like warfarin or levothyroxine), the range tightens to 90% to 111% to ensure safety.
Pharmaceutical vs. Therapeutic Equivalence
Confusing terms? You’re not alone. Pharmaceutical equivalence means two drugs have the same active ingredient, dose, and form (like tablets or injections). But they might differ in inactive ingredients (fillers or dyes). This doesn’t guarantee the drugs work the same in your body.
Therapeutic equivalence is the gold standard. It requires both pharmaceutical equivalence and bioequivalence. The FDA assigns "AB" ratings to generics that meet this standard. For example, a generic metformin with an AB rating can be substituted for the brand-name Glucophage without concerns. If a drug lacks this rating (like some topical creams), pharmacists can’t automatically switch it.
The Orange Book, published by the FDA, lists all approved generics with their therapeutic equivalence codes. This is the go-to reference for doctors and pharmacists deciding if substitution is safe.
Real-World Evidence: Do Generics Work?
For most medications, the answer is yes. A 2020 FDA analysis of 2,070 generic drugs found 98.7% had AUC ratios within 90% to 110% of brand-name versions. In everyday practice, independent pharmacists report no significant differences for 87% of patients switching to generics (National Community Pharmacists Association, 2022).
But exceptions exist. Levothyroxine (for thyroid issues) is a common example. Some patients report symptoms when switching between generic brands, though studies show this is rare. The FDA now requires stricter bioequivalence testing for thyroid drugs-each generic must match the exact brand used in clinical trials. Many states also require pharmacists to use the same manufacturer once a patient is stabilized.
Adverse event reports are minimal. In 2022, only 0.3% of medication-related issues reported to the FDA involved generics, proportional to their 90% market share. This data confirms that for the vast majority of drugs, bioequivalence standards work.

Why Bioequivalence Matters
Without bioequivalence standards, generic drugs wouldn’t exist. The Hatch-Waxman Act of 1984 created the pathway for generics by requiring bioequivalence testing instead of new clinical trials. This saved the U.S. healthcare system an estimated $2.2 trillion over the past decade.
For patients, it means lower costs. A generic prescription saves an average of $313 per fill (AARP, 2023). For chronic conditions like diabetes or hypertension, this adds up to thousands saved yearly. Globally, the generic market is worth $400 billion, with bioequivalence standards enabling this growth.
Regulatory differences exist. The European Medicines Agency (EMA) sometimes uses wider equivalence ranges for highly variable drugs (75% to 133%), while the FDA is stricter. But the core principle remains: ensure safe, effective alternatives to expensive brand-name drugs.
Frequently Asked Questions
Are generic drugs as safe as brand-name drugs?
Yes, for the vast majority. The FDA requires generics to meet the same quality, safety, and efficacy standards as brand-name drugs. Bioequivalence testing ensures they deliver the same active ingredient at the same rate. Only in rare cases (like some narrow therapeutic index drugs) might switching cause issues-but even then, regulators have specific safeguards.
Why do some people say generics don’t work as well?
Placebo effects or unrelated health changes often explain this. A 2023 Consumer Reports survey found 78% of patients were satisfied with generics versus 82% for brands. The largest gap (12 points) was for antiepileptic drugs, where small differences in blood levels matter. But for most medications like antibiotics or statins, no meaningful difference exists. Always talk to your doctor or pharmacist if you notice changes.
How does the FDA ensure generics are equivalent?
Through rigorous bioequivalence studies. Manufacturers must test their generic against the brand-name drug in healthy volunteers. The FDA reviews data on Cmax, AUC, and tmax to confirm results stay within 80%-125% (or tighter for high-risk drugs). They also inspect manufacturing facilities and require ongoing quality checks. Over 1,200 generic applications are reviewed yearly, with 98.7% meeting standards.
Can I switch between different generic brands?
For most drugs, yes. Generics with the same AB rating are interchangeable. However, for thyroid medications like levothyroxine, some states require staying with one manufacturer once stabilized. Always check with your pharmacist-especially if you’ve noticed changes in how you feel after switching.
What’s the difference between pharmaceutical and therapeutic equivalence?
Pharmaceutical equivalence means two drugs have identical active ingredients and dosage forms. Therapeutic equivalence goes further: it requires bioequivalence too. Only drugs with therapeutic equivalence (marked "AB" in the FDA’s Orange Book) can be safely substituted. For example, a generic aspirin tablet is both pharmaceutically and therapeutically equivalent to brand-name aspirin.





Brendan Ferguson on 6 February 2026, AT 13:38 PM
As a pharmacist with over a decade of experience, I can confidently say that bioequivalence standards are rigorously enforced to ensure generic medications are just as effective as brand-name drugs. The FDA requires that generics deliver the same active ingredient in the same amount and at the same rate as the original drug, measured through Cmax, AUC, and tmax parameters. This 80-125% range isn't arbitrary-it's based on extensive clinical data showing that variations within this margin don't impact therapeutic outcomes for most patients. For instance, common medications like statins or antibiotics have been used interchangeably for years with no significant difference in efficacy. While there are rare exceptions for drugs with narrow therapeutic windows, the vast majority of generics are safe and effective alternatives. It's important to remember that these standards exist to protect patients while making healthcare more affordable. Always consult your healthcare provider if you have specific concerns, but rest assured that the system is designed to prioritize your health and safety.